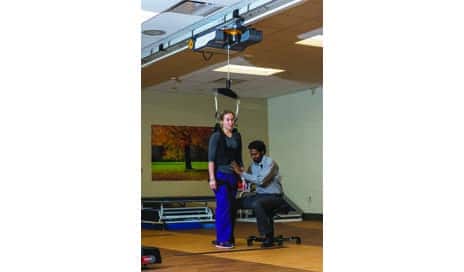
A dynamic overhead harness and railing system allows the safe practice of high-risk activities during mobility. When patients can learn from their mistakes without causing physical harm, they may acquire skills they can take with them after they leave the clinic.
by Robert Walters, PT, MBA
Many therapists spend at least part of their time with patients teaching them a valuable skill. It may involve explaining to the patient how to use correct body mechanics to reduce the strain on the patient’s back, or clarifying the right technique for going up and down stairs following a total knee replacement. Regardless of the topic, when therapists teach, they don’t expect their patients to do things perfectly the first time. Failure is, initially, par for the course and provides the clinician an opportunity to give appropriate feedback and various types of practice along the way to help our patients ultimately succeed.
Yet when it comes to teaching patients how to avoid a fall, failure can result in harm for both the patient and the clinician, not to mention reflect poorly on the overall safety of the hospital or clinic. Therefore, it is not surprising that many health systems have developed robust fall prevention programs focused on addressing the various factors that may lead to a fall. These programs often include implementing universal fall precautions, completing standardized assessments of fall risk factors, care planning around the identified risk factors, and conducting post-fall root cause analysis. Without question, these are all valuable practices that can help keep patients and clinicians safe. Unfortunately, prevention programs can’t eliminate all the external environmental factors a patient might encounter outside of the hospital or clinic, such as the unseen crack in the pavement or the rambunctious child bumping into them at the grocery store.
Similarly, many clinics and hospitals require the use of gait belts when clinicians are ambulating or working on transfers with their patients. Obviously, gait belts can be a valuable safety tool. However, when a patient starts to fall, and the therapist tugs on the gait belt to correct the patient’s posture, the patient is not provided the opportunity to intrinsically feel the boundaries of their limitations and associated consequences of exceeding them. The inherent value of learning by failing can be seen when toddlers are first learning to walk. In fact, there is so much more falling involved than walking that research has been done to study why toddlers decide to abandon crawling all together. But over time, the child builds strategies and becomes more aware of where their body is in space through the natural feedback that the falls provide.
First Attempt In Learning
Given that fall prevention programs can’t always prepare the patient for the unexpected, and that we know the human body is capable of responding and adapting to meet challenges, therapists at John Muir Health are exploring the value of having their patients’ failures be their First Attempt In Learning how to move safely. Inside the facility, a dynamic overhead rail and harness system has been installed that allows clinicians to push the balance envelope and lets the patient experience failure in order to safely learn from their mistakes. The rail system is comprised of 142 feet of track that winds through designated areas within the facility’s 7,000-square-foot rehabilitation center. Each of these areas allow patients to practice various functional activities and challenge their proprioceptive boundaries, while keeping the patient and therapist safe from harm.
The rail system starts over a wide high/low mat table. Therapists often use this area to work on sit-to-stand transfers with their more physically challenging patients. Because the harness system is dynamic, if a patient lacks the strength to transition from sit to stand independently, the therapist can offload just as much of the patient’s weight as needed so they are challenged yet able to move through the range. As the patient grows stronger, the therapist can document the reduction in assistance from the rail system to demonstrate objective progress.
For patients who routinely lean too far forward and stumble, the therapist can set the rail system to limit how far the patient will drop should they begin to fall. As a result, clinical staff members have observed that after failing on their own, many patients begin to develop an intrinsic awareness of “how far forward is too far,” and they make the appropriate corrections. Conversely, we have observed the harness help the patient who is reluctant to bring their “nose over toes” when initiating standing. Often, this fear results in the patient compensating by standing up with their weight through their heels and falling back on to the mat or chair. However, when the patient is in the harness, and trusts the system will catch their fall, therapists may observe the patient’s confidence improve and they begin to shift their weight anteriorly, resulting in a smooth and appropriate transition into standing.
Floor Transfer Techniques
Teaching floor transfer techniques is a training activity that causes trepidation among many patients and therapists. Often, patients who might need the practice the most are also the most challenging to get down to the floor safely. This leaves the therapist questioning how much help the patient will require to get back up. The rail system at this facility has been designed to pass through an area of “open space” where patients and clinicians can work to alleviate these fears. To get patients safely to the floor, therapists can engage a setting that automatically slows the rate of descent as they near the floor. This reduces the likelihood of injury for both the patient and clinician, and can be done with the work of only one therapist, thereby maximizing the efficiency of other staff members.
When the patient is ready to practice moving from floor to standing, the therapist can dial in just the right level of assistance that the rail system needs to provide so that the patient is appropriately challenged, and can learn safely from their mistakes. If there is one specific phase of the transfer where the patient needs the most training, repetition can be performed quickly, and with the patient’s body weight reduced to help offset fatigue.

Gait belts can be a valuable safety tool. However, when a patient starts to fall, and the therapist tugs on the gait belt to correct the patient’s posture, the patient is not provided the opportunity to intrinsically feel the boundaries of their limitations and associated consequences of exceeding them.
Gait Training
The harness system is used most frequently in the gait training section of the rehab center. This is an area with a straight portion of overhead track, 50 feet in length. Underfoot, there is a designated pathway with markers every 10 feet on the floor to help therapists quickly determine the distance the patient has walked. Gait training while in the harness provides the same benefits as described with floor recovery and sit-to-stand training when it comes to safely learning from failure. Further, the patient can focus solely on their gait mechanics without being distracted by maneuvering an assistive device, such as a walker, at the same time. While the patient is walking in the harness, therapists are free to use their hands for something more therapeutic than holding a gait belt, such as the multitude of manual facilitation techniques that lower-level patients may benefit from in walking. With the patient support coming from above rather than a frame surrounding the patient, clinicians can facilitate the patient from any angle and use the harness while the patient practices stairs, uneven surfaces, or even running.
For higher-level patients who may not routinely fall with walking or transfers, yet have a certain level of unsteadiness with movement, the harness system allows therapists to take these activities one step further. A reference is made earlier in this article to one of the limitations of typical fall prevention programs—that they are unable to replicate the unexpected balance disturbances that occur during the course of everyday life. Once outside the hospital or clinic, there are any number of scenarios that require patients to use quick and timely corrective postural adjustments to remain upright.
Therapists at John Muir Health can replicate these scenarios with patients while the patients are in the harness. This is done by giving the patient a random nudge from the side while walking or a bump from behind while practicing going up and down a curb. Additionally, therapists can work specifically on balance adjustments in any direction by having the patient lean into the therapist and the therapist subsequently—and suddenly—remove their support. Therapists have not traditionally been in the practice of causing patients’ falls, but when correctly supported, this type of training can be very useful in preparing patients for the real world they will encounter. RM
Robert Walters, PT, MBA, is Director of Inpatient Rehabilitation Services at John Muir Health in the San Francisco Bay Area. For more information, contact [email protected].