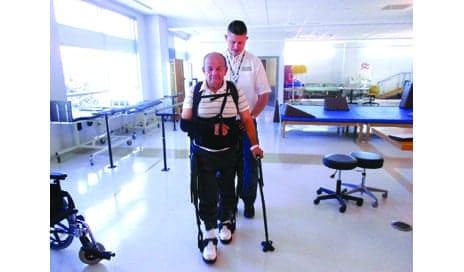
Providing an opportunity for high-repetition stepping can help patients recovering from stroke to build their walking endurance.
by Kirk D. Endersby, PT, NCS, and Eric Schwelke, CPO, LPO
Regaining the ability to walk after having suffered a cerebrovascular accident (CVA) or stroke is probably one of the most, if not the most, frequently expressed goals when patients begin their acute rehabilitation program. “I want to be normal again,” “I want to be able to do the things that I used to.” Understandably, to many stroke patients, walking again is a vital component of being “normal.”
Facing the challenge of regaining function after a stroke is something Americans are facing in increasing numbers. According to American Stroke Association statistics, stroke is the number one cause of disability in the United States with approximately 795,000 new or recurrent strokes occurring each year.1 While mortality rates from stroke have declined somewhat in recent years, there are more people than ever living with the detrimental effects of CVA. This includes impairments that limit the ability to walk.
At Kessler Institute for Rehabilitation, located in West Orange, Chester, and Saddle Brook, NJ, the challenge of getting stroke patients back on their feet is addressed by the interdisciplinary team each day. More than 1,400 patients were treated by the Stroke Team within the three main inpatient hospital sites during this past year. Thus, there are many opportunities to address gait training and other functional activities with these clients who have varying degrees of impairment.
While there are some who will not be physically ready to ambulate safely during their acute rehabilitation stay (approximately 3 weeks), many of the facility’s clients achieve household or community ambulation status. Even so, these patients frequently require assistance of a caregiver to do so safely at home. Gait training primarily is addressed by the physical therapist (PT), but success in this endeavor requires the support and contribution of an interdisciplinary team of healthcare professionals, including the physiatrist, nurse, occupational therapist, orthotist, and the patient’s family.
Case Study
To get a better idea of what gait training may include for a stroke patient at Kessler, following is the acute rehabilitation pathway of Juan, a patient recently treated by the Stroke Team.
Juan is a 65-year-old male who worked as a delivery man for a local company. Prior to his stroke, he lived with his wife and adult daughter in a private, one-story home with five stairs to enter. Juan’s daughter describes her father as “a very independent and active man who was always busy doing something around the house.”
Juan suffered a left internal capsule infarct that affected his strength and sensation on the right side of his body. His past medical history was significant for diabetes mellitus, hypertension, and dyslipidemia.
Five days after initially being diagnosed at a local acute care hospital, Juan was transferred to Kessler Institute to begin his acute rehabilitation. Upon initial evaluation in physical therapy, Juan was found to have the following impairments:
Manual Muscle Testing: Right upper-extremity strength: 0/5 at shoulder, elbow, wrist, and hand. Trace scapular retraction noted.
Right lower-extremity strength: hip flexion: 2/5, hip abduction: 2-/5. knee flex: 3+/5, knee extension: 3+/5, ankle dorsiflexion and plantarflexion: 0/5.
Range of Motion
Passive range of motion of the right upper and lower extremities was within normal limits.
Left upper and lower-extremity active and passive range of motion: within normal limits.
Tone: Low tone noted in the right upper extremity and lower extremity, but more so in the upper extremity. 1+ ( MAS) rating given to right hamstring and hip adductor tone.
Low tone noted in the right lateral trunk flexors (noted in sitting)
Sensation: Impaired sensation to light touch noted in the right upper and lower extremities.
Impaired proprioception noted at the right ankle.
Functional movement: Bed mobility: short sit to and from supine with moderate assistance for right lower-extremity management, trunk support, and safety.
Transfers: Sit to stand from wheelchair-level with moderate assistance for balance and safety. Stand pivot transfer from wheelchair to mat on the right or left side: moderate assistance.
Ambulation: 30 feet with right dorsiflexion ace wrap, narrow base quad cane, limited by right lower-extremity fatigue.
Stairs: four (6-inch) steps with one rail and minimal assistance for balance and right lower-extremity placement.
Other observations: mild dysarthria, right-sided facial droop, static standing up to 1 minute with minimal to moderate assistance, limited by fatigue. Patient was well-motivated and eager to participate.
Initial Phase of Gait Training – Lead-ups
With impairments in the right lower extremity, strength, and sensation, Juan had difficulty maintaining stance control on the right. Gait training interventions during initial sessions included focus on closed-chain exercises in standing with use of a mirror for visual feedback to retrain Juan’s body to sense and use of the right lower extremity for support. Exercises such as left heel lifts or stepping in various directions and onto various surface heights were used to progress demand on the right lower extremity.
Manual cues to the right quadriceps and right gluteus muscles were used to facilitate stabilization in the limb. Postural cues to abdominals and/or right lateral trunk flexors were used to promote upright posture. Efficient standing posture was further aided by the use of a dynamic sling for the right upper extremity. This sling allows the arm to be supported at the side of the body instead of pulling the trunk into flexion.
The primary goal of this first phase of training was to help Juan re-establish a sense of balance and begin to trust the right lower extremity again for support.
Next Phase of Gait Training: Stepping
Once some confidence with right stance was accomplished, progression toward stepping with the right limb was initiated. The right ankle was supported with a dorsiflexion ACE wrap to assist with foot clearance in the absence of active dorsiflexion. An elevated, rolling bedside table was used for left upper-extremity support at the elbow during the initial stages of gait training. This provided the patient with added support and confidence to begin to rely on the right lower extremity for stance support again. The table also allows for a more fluid gait pattern by providing “rolling support” as opposed to a segmented three-point gait pattern with a cane. As Juan demonstrated improved confidence with this set-up he was progressed to the more functional device for home—in this case, a narrow base quad cane.
Innovative Therapy Options
To supplement what might be considered a more traditional gait training approach, utilization of other available technologies served to enhance the relearning process. A standing frame was used to provide longer periods of weight bearing for Juan. By stabilizing the lower extremities, Juan was also able to participate in various reaching activities designed to promote active trunk range of motion and strengthening. Juan was also able to build his upright tolerance.
A robotic exoskeleton was used as a means to provide Juan with high-repetition stepping in a safe, supported frame. In conjunction with the Kessler Foundation Research Center, Juan was able to participate in a research study that enabled him to use the device during his inpatient stay. Juan was measured and fit with the device which was programed and guided by his physical therapist. This particular device can be set up to provide total lower-extremity assistance for stepping or be programed to only provide the needed assistance to the limb in need. Juan was set up to control his own left lower extremity and receive assistance for the right lower extremity as needed to facilitate mass practice with the functional activity of gait with an assistive device (in this case, a narrow base quad cane). With use of the device, Juan was able to ambulate up to 1,200 steps during a 1-hour PT session. The device was useful in enabling Juan to build his walking endurance, and the guided stepping promoted symmetry of gait between the right and left sides.
Body weight-supported treadmill training was used as another means of providing massed practice with stepping in a safe environment. With the support of a body harness and frame, Juan was free to step and walk without the fear of falling. When ambulating over the treadmill with the support, the PT was able to use manual cues to assist the right lower extremity (hamstrings, ankle) with improved clearance and foot placement. After training on the treadmill, Juan would then ambulate overground, still supported in the device. The device enabled Juan to “experiment” in a safe way with ambulation to try and relearn the sensation of walking and using the right lower extremity.
As Juan progressed in his gait training, he began to demonstrate signs of active return in his right ankle. With trace muscle activity noted in the anterior tibialis, use of a lower-extremity functional electrical stimulation (FES) orthosis was initiated. Use of the device not only enabled Juan to exercise his leg in sitting, but when combined with a heel switch, enabled Juan to actively dorsiflex his foot during gait training. This built encouragement for Juan. However, his leg strength was still weak, and with his inpatient time nearing completion, it was clear Juan would need the added support of an orthosis to be able to ambulate safely upon his return to home.
Lower-Extremity Bracing
Juan was considered to be an orthotic candidate during the first week of his inpatient rehab stay and was referred to the Kessler brace clinic after his primary PT trialed various bracing options. The lower-extremity brace clinic team is composed of a physiatrist, an orthotist, and a physical therapist who meet weekly to evaluate clients’ bracing needs. At the time of referral to brace clinic, Juan presented with 0/5 in both right ankle plantar and dorsiflexion. Quadriceps strength was rated at 3+/5. Juan’s gait was analyzed with use of a dorsiflexion ACE wrap to enable foot clearance with gait.
A prefabricated, standard trim ankle-foot orthosis (AFO) was also trialed. For this patient, with a history of diabetes, the long-term use of a prefabricated orthosis would be contraindicated as it posed a skin breakdown risk due to the lack of an intimate orthotic fit. A more prudent course would be the use of some type of custom molded ankle foot orthosis if the anticipated use would be more than 6 months. The device of choice would be the standard molded AFO to secure the ankle foot complex in neutral and lock out any abnormal tone. To protect against skin irritation, a soft molded interface was included.
Since increased AROM is expected, an articulated, custom molded AFO with adjustable ankle joints would be optimal, initially locking out ankle motion and having sequential adjustments made by the orthotist to account for the returning AROM. This would be the ideal situation, but unfortunately, insurance payment considerations did not allow for this orthotic device to be chosen. Looking further down the road for Juan, if most of his AROM returns, his tone reduces, and some ankle weakness remains, a carbon fiber dynamic AFO may be trialed as well. The brace clinic team decided that Juan would be best served by being fit with a custom, standard trim MAFO.
For patients similar to Juan, recent advances in pressure mapping technology have enabled clinicians to collect objective data while gait training their patients, including patients with stroke. For example, portable pressure mapping surfaces or electronic walkways are being used to collect data in real time about gait parameters such as gait speed, step and stride length and width, and even specifics regarding distribution of weight through the foot. This technology can assist clinicians with objective assessment and goal setting, and has been used by some to justify the need for skilled care. For patients affected by stroke, this tool can help in their quest to achieve a symmetrical gait pattern from side to side, and ultimately help to improve patient balance and safety.
In addition to the gait training interventions and considerations noted above, it should also be noted that a key factor in Juan being able to return home as an ambulator was his family support at home. Even with orthotic support at the right ankle/foot and a steadily improving gait, Juan continued to require some hands-on assistance for lingering balance issues related to ongoing weakness and incomplete sensory awareness of the right lower extremity. Juan’s daughter came in for several gait training sessions to learn how to safely guard Juan at home.
Returning to Home
Upon leaving Kessler, Juan was able to perform the following:
Transfers: Sit to stand with close supervision for safety with right foot setup and for stand-pivot transfers, close supervision to contact guard assist for balance, and safety with right foot placement.
Mat/bed mobility: short sit to and from supine with modified independent.
Ambulation: >200 feet with narrow base quad cane, right standard trim MAFO, right dynamic arm sling with contact guard to minimal assistance on level surfaces.
Stairs: negotiates 13 (7-inch) steps with one rail with contact guard to minimal assistance needed for balance and safety.
Through a gait training program supplemented by the latest in assistive technology and a skilled orthotics team, Juan was able to return home from his acute rehabilitation stay at Kessler. He planned to continue with outpatient therapy to continue in his quest to be an independent ambulator. Developments in assistive technology have enabled therapists to assist stroke patients onto their feet earlier, for longer periods of time, and have given therapists tools to provide massed practice for gait recovery. With appropriate support and the recommendations of a skilled orthotics team, patients are enabled to continue these relearned gait skills safely at home. Getting back to “normal” may take more time than allotted in a relatively short inpatient rehab program, but it is more likely to be accomplished with the innovative treatment plans provided by an interdisciplinary team. RM
The authors wish to thank Barbara Garrett, PT, for her contributions to this article.
Kirk D. Endersby, PT, NCS, earned a bachelor of science in physical therapy from University of Illinois-Chicago in 1996. For the last 18 years, Endersby has worked at Kessler Institute for Rehabilitation, West Orange, NJ, as an advanced clinical specialist, primarily treating stroke and brain-injured patients. He is a member of the American Physical Therapy Association.
Eric Schwelke, CPO, LPO, earned a bachelor of arts in physical anthropology from State University of New York at Buffalo in 1976, and a bachelor of science in prosthetics and orthotics from New York University in 1979. Schwelke was in private practice in New York for 24 years and was owner of Ultrapedics Ltd. He was also a consultant in P&O as the owner of Bionic Resources LLC, Member of the American Academy of Orthotists and Prosthetists, and certified in numerous systems for upper and lower prosthetic devices. Schwelke currently is director of Kessler Orthotic & Prosthetic Services Inc, Livingston, NJ. For more information, contact [email protected].
Reference
- American Heart Association Statistical Update. Heart Disease and Stroke Statistics-2015 Update. Available at: http://circ.ahajournals.org/content/131/4/e29. Accessed October 27, 2015.