Compiled by Debbie Overman, Associate Editor The myriad of equipment available to rehab therapists, as well as the purposes for which it is used, is as varied as the therapists themselves. Depending on each patient and the therapist’s creativity, the equipment can be used in concert with specific exercise and conditioning regimens to help aid recovery and relieve pain from surgery or cancer treatment, gain function and range of motion following stroke or injury, learn new skills in order to live with a new reality as the result of a spinal cord injury, and more. Managers and clinicians from five rehabilitation facilities share the equipment they use most often to build strength and conditioning and meet other specific rehab goals. They also spotlight technologies that help maintain a competitive advantage and discuss the importance of trialing equipment prior to purchase.
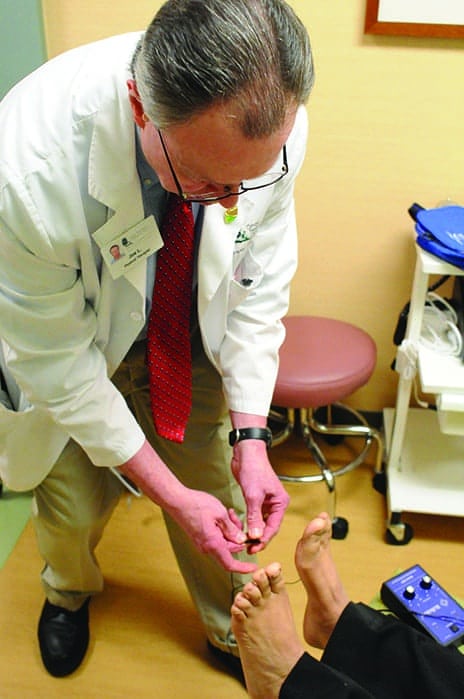
Joe L’Abbe, PT, CLT, Physical Therapist, Cancer Treatment Centers of America, Chicago, uses an electrical stimulation device to help reduce pain for a patient with chemotherapy-induced peripheral neuropathy.
Cancer Treatment Centers of America, Chicago
Cancer Treatment Centers of America (CTCA) Chicago is part of a comprehensive network of hospitals and outpatient care centers that offers individualized exercise programs and services to help oncology patients before, during, and after treatment. This support may include helping patients improve range of motion (ROM), addressing all forms and causes for pain, addressing neuropathy (weakness, numbness, and pain caused by nerve damage) with electrical stimulation, improving balance, and minimizing fatigue and weakness, says Tara Alaichamy, PT, DPT, CLT, manager of oncology rehabilitation services at CTCA. The strength and conditioning equipment used in the physical therapy gym by CTCA therapists for these purposes include upper body ergometers and low-weight pulley systems, especially with postoperative breast cancer patients, to help patients who are at risk for poor posture, decreased upper body strength, and limited mobility. Mid-back strengthening (specifically mid and lower trapezius, and serratus anterior) and upper body mobility (targeting range of motion improvement for the shoulder/glenohumeral joint) that the ergometer provides helps increase strength and improve overall range of motion. “Many oncology patients, especially those experiencing weakness or fatigue associated with chemotherapy or radiation therapy, also benefit from the use of a recumbent stepper,” Alaichamy explains. Requiring the user to engage many muscles used in basic daily tasks and simple chores, the pumping action of a recumbent stepper is a great option for providing comfortable positioning while patients perform low-impact, endurance exercises, Alaichamy adds. A bioimpedance spectroscopy device, which can be valuable to provide objective measurements to assist with lymphedema diagnosis and management, is among the equipment CTCA therapists use to help maintain a competitive advantage or attract referrals. Alaichamy explains that CTCA therapists often perform limb volume measurements with these devices before patients undergo lymph node and breast surgeries to establish a baseline for postsurgical care. “When significant changes in pre- and post-surgical measurements are identified, the patients’ therapist can immediately notify their physicians to discuss other lymphedema management options,” Alaichamy says. Another diagnostic tool used by the CTCA care team, including rehabilitation therapists, is a body composition analyzer. This tool helps monitor muscle mass, total body water, and fat to help identify patients who may benefit from immediate rehab intervention. If a patient exhibits significant muscle loss, a referral to rehabilitation services for strength and mobility support can be an important step to help improve and maintain quality of life during and after treatment. Lastly, CTCA therapists frequently use a prescription-only electrical stimulation device to help reduce neuropathy-related pain. Chemotherapy-induced peripheral neuropathy can be one cause of this type of pain. Combined with a thorough assessment, education, and exercise, the electrical stim device can be a helpful alternative to pharmaceutical pain medications and reduce pain associated with chemotherapy-induced peripheral neuropathy. “Equipment features that provide objective data for functional outcomes are always important for monitoring patients’ progress and motivating them,” Alaichamy notes. Any patient undergoing rehabilitative care can have complex needs, including oncology patients, and so having adaptive features is also a must-have. When looking for a recumbent stepper, for example, it can be helpful to choose equipment that can provide many options for use. Some recumbent steppers allow users to isolate arm-pumping action, which can be help for improving upper body strength and ROM in breast cancer patients. “Understanding the needs of cancer patients is one of the most important first steps in evaluating and researching conditioning and training equipment,” Alaichamy shares. “Once a need is identified, the CTCA team works collaboratively to review all options and select the one that has the best potential to help patients.”
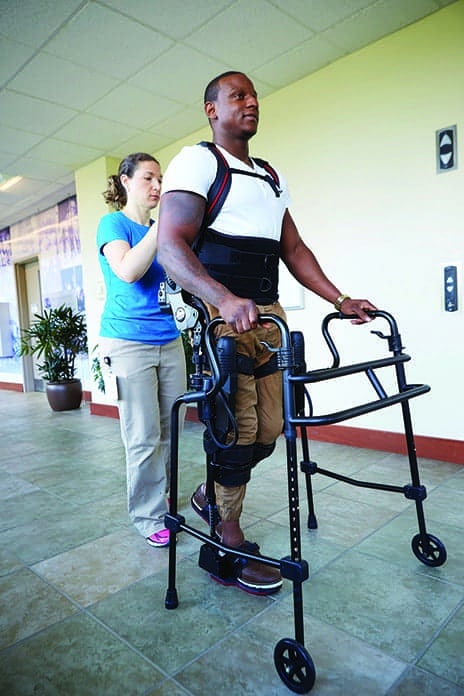
Good Shepherd was one of the first rehabilitation facilities in the United States to receive an exoskeleton that is designed as a wearable robotic device to allow people with lower extremity paralysis or weakness to stand and walk.
Good Shepherd Rehabilitation Hospital
Good Shepherd Rehabilitation Hospital (GSRH), Allentown, Pa, specializes in meeting the complex needs of patients who have had a catastrophic accident, injury, or illness. Patients travel to Good Shepherd from throughout the United States and beyond, and the therapy team develops a customized treatment plan for each one based on their goals and diagnosis, says Sue Golden, PT, NCS, neurorehabilitation director. The recumbent bike, NuStep, and Uppertone are often used to help patients build strength and improve conditioning. “We find this combination effective because therapists cannot always replicate the same movement over and over again using their hands for strengthening. Patients need many repetitions of movement—the correct movement—not only to gain strength but also to promote neuroplasticity and hardwire new movements,” Golden explains. Other technology used at Good Shepherd include the Bioness H200, a neuroprosthetic system designed to help patients with upper-limb paralysis regain hand control and improve function; the Ekso Bionics Exoskeleton, a wearable robotic device engineered to allow people with lower extremity paralysis or weakness to stand up and walk; and a warm water therapy pool, which helps to increase circulation, respiratory rate, muscle metabolism, strength, flexibility, and movement while reducing pain through decreased weight-bearing and joint stress. “Since we treat patients with a variety of abilities due to motor control and musculoskeletal changes at Good Shepherd, it is very important that the equipment we use have adaptive features in order to give patient feedback and data,” Golden shares. There are several reasons for this, she says. First, there are times when patients need to be shown that improvement is needed. Second, it helps to substantiate progress. Feedback features on devices like the Ekso alert the patient when they are performing something correctly or give them cues to perform in a better movement or pattern. With this in mind, Golden explains, if the therapists at GSRH feel a piece of technology has the potential to help patients, they request a staff demonstration session and the opportunity to trial it. The facility’s Product Committee also reviews it. Depending on the cost, a number of factors are considered in the decision to adopt new equipment at Good Shepherd. “These include how many patients it can impact, customer service and training, ease of use for clinical integration, staff input, and whether or not we need to make structural changes to accommodate it. We also identify staff super users to maintain and train new staff and help promote its use,” Golden explains.

The Intelligently Controlled Assistive Rehabilitation Elliptical (ICARE) trainer is a fully integrated system developed at Madonna Rehabilitation Hospitals’ Research Institute. ICARE provides a safe, effective method for addressing walking and fitness goals of patients with neuromuscular disorders resulting from stroke, TBI, partial SCI, and other injuries or diseases.
Madonna Rehabilitation Hospitals
Madonna Rehabilitation Hospitals is a comprehensive hospital-based rehabilitation facility that serves both inpatient and outpatient clientele across the continuum of care. It includes a 24-acre campus in Lincoln, Neb, as well as a second 20.6-acre campus in Omaha that opened in the fall of 2016, according to Michele Ohlmann, PT, director of inpatient therapy. Madonna specializes in complex medical, traumatic brain injury, spinal cord injury, pulmonary conditions, severe stroke, other neurological conditions, and pediatric rehabilitation. Madonna also owns ProActive, a medically based health, fitness and wellness facility that provides access to medical, therapeutic, and educational fitness needs for adults of all abilities. The equipment frequently used within the inpatient setting for building strength and conditioning include the ICARE (motor-assisted elliptical), Nu-Step, Moveo tables, and upper body ergometers. The technology is useful to patients for the ease of transfer to/from the devices and to challenge cardiorespiratory fitness and strength, Ohlmann explains. The ICARE also allows patients to work on their walking and balance in an upright position. “This is vitally important for patients receiving care in the rehabilitation setting, who often have difficulty walking and poor balance due to weakness or movement control problems. Since both inpatients and outpatients often have limited therapy time, treatment approaches— such as the ICARE—simultaneously address multiple goals,” she says. The ICARE is a motor-assisted elliptical that promotes movements closely simulating joint motions and muscle demands of walking. Additionally, the ICARE provides customizable levels of motor-assistance to the pedals and external body weight support, enabling users to train without physical assistance from clinicians. “Other gait training approaches, requiring a clinician to repeatedly lift and advance a patient’s leg, can lead to clinician injuries. ICARE helps us protect one of our most valuable assets—our experienced clinicians,” Ohlmann shares. The ICARE also helps therapists at Madonna Rehab maintain a competitive advantage as it is an affordable robotic device designed to allow clinicians to customize treatments to the unique needs of patients while challenging muscle demands and cardiorespiratory fitness. Parameters such as training speed, level of body weight support, and amount of external motor-assistance have been shown to influence lower extremity muscle demands and cardiorespiratory fitness (eg, heart rate, systolic blood pressure, perceived exertion). “We use the ICARE in our inpatient, outpatient, and medical fitness settings. Additionally, individuals have purchased the ICARE for home use,” Ohlmann notes. Patients, families, and clients review online information regarding product use and technology options when making decisions regarding admission to Madonna’s inpatient rehabilitation programs, in order to participate in rehabilitation using technology to advance and progress functional outcomes following injury. Numerous robotic/exoskeleton devices for functional training use are on hand at Madonna to assist patients with their goals. “Having product features that engage and motivate patients is an important tool and strategy for functional improvement. With this in mind, we consider any adaptive features that would allow use for a variety of impairments and/or limitations before purchasing new technologies or therapy equipment. Collaboration between clinicians, patients, caregivers, and the multidisciplinary team of researchers and engineers in Madonna’s Research Institute fosters a commitment to develop affordable, customized, practical adaptive features to allow the most complex patient access to equipment,” Ohlmann adds. Prior to purchase of conditioning and training equipment used at the facility, therapists work collaboratively with vendors and manufacturers regarding possible trials or demonstrations, and consider such factors as vendor relationships, installation ease, and access to service in their decision-making. They also work closely with colleagues in Madonna’s Research Institute and at ProActive, to advance new technologies and ensure that a broad range of devices addressing the needs of individuals throughout their rehabilitation journey and return to the community are available.

Individuals are at a higher risk of reinjury if they return to work without proper work conditioning. PTWI physical therapist Marc Schoettle guides a patient through job-specific exercises as part of a Work Ready program to help patients recover properly and return to work after injury.
The Physical Therapy and Wellness Institute
The Physical Therapy & Wellness Institute (PTWI) is a private outpatient physical therapy clinic in a middle-income suburban area outside of Philadelphia that serves primary a general orthopedic and postsurgery population with vestibular, TMJ, and pelvic floor specialties, according to Christian Barrett, PT, DPT, PTW Lansdale Clinical Supervisor. PTWI uses a variety of bi-angular strengthening equipment built with the purpose of adapting to a variety of body types to provide a uniform, comfortable, and safe environment when strength training in the clinic. “PTWI often receives direct referrals for aquatic therapy using our two deep-water therapeutic pools that are heated to 94 degrees,” Barrett says. In these pools, therapists can develop programs to help patients unload joints, increase heart rate for chronic pain, and perform buoyancy-assisted exercises to aid in restoring ROM. “In eight of our other facilities PTWI provides anti-gravity treadmills designed with unloading technology to help patients walk or run from 20% to 100% of their body weight,” Barrett adds. When it comes to products that help motivate patients, assist those with limited function, or use assistive devices, it is PTWI’s goal to perform objective measures on a weekly basis for its patients in order to provide motivation through positive reinforcement. “Our clinics are accessible for all patients as we have an automatic door opener for easy access to the clinic. We also have a hydraulic lift for one of our therapeutic pools for patients who are unable to use stairs and a ladder to access our pools,” Barrett explains. Conditioning and training equipment appropriate for PTWI’s rehab patients is selected and trialed via a dealer with which it has a working relationship. “We also value input from our therapists when it comes to equipment selection and will always take their opinion and needs into consideration when selecting equipment for the clinic,” Barrett adds.
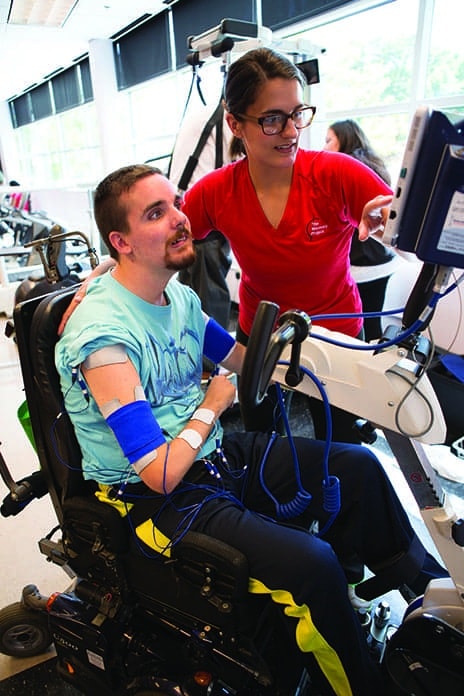
The Recovery Project offers its clients state-of-the-art functional electrical stimulation equipment, which is utilized in conjunction with evidenced-based treatment approaches.
The Recovery Project
The Recovery Project (TRP), Livonia, Clinton Township, and Lansing, Mich, provides evidence-based progressive and effective physical, occupational, and speech therapies to clients who have suffered spinal cord, neurological, and traumatic brain injuries. It builds unique therapy programs designed to directly help every client meet his or her specific goals, shares Polly Swingle, PT, GCS, CEEAA, chief executive officer and co-owner. Strength equipment used at TRP includes functional electric stimulation (FES) to help improve strength, motor control, and sensation in clients diagnosed with a central nervous system injury or disease. FES RTI arm and leg cycles, a gait trainer, and the Xcite (FES with functional activities), are also utilized, as well as blood flow restriction (BFR) training to facilitate strengthening. BFR is a training strategy involving the use of cuffs placed around a limb during exercise, which maintains arterial inflow to the muscle while preventing venous return. Research on traditional loading requirements for hypertrophy (muscle growth) during weight lifting suggests loads heavier than 65% of an individual’s one rep max must be used to create hypertrophy gains. “Clients with neurological diseases or injuries are unable to load their bodies with this much of a load. Therefore, BFR is used to facilitate a strength gain,” Swingle explains. The Red Cord Suspension Training system, which allows a client to use their own body weight as resistance or unweight the body to enable exercise to be completed in a gravity-minimized environment, is also used, as well as traditional forms of pulley systems, weight machines, bands, and free weights, Swingle adds. Strength and conditioning used at TRP include FES for cardiovascular conditioning. “The client is moving their large muscles in a functional pattern, which in turn results in a cardiovascular effort, an increase in heart rate, and contraction of the stimulated muscles. Typically, individuals with a SCI, TBI, CVA, MS, etc, have difficulty increasing their heart rate and training their muscles for endurance. FES cycling is a tool that can assist with this,” Swingle notes. Since The Recovery Project is a specialty clinic that treats clients with neurological diseases or injuries, all of the treatments it provides are based on the newest clinical evidence that supports neuroplasticity and recovery. “The evidence supports utilizing FES for anyone with a central nervous system injury, and the equipment we have on-site that makes us maintain a competitive advantage or attract referrals are our RTI 300 FES arm and leg cycles, FES RTI 600 gait trainer, and Xcite (FES for functional activities),” Swingle adds. Evidence also supports utilizing a body weight support system to facilitate recovery of gait following a central nervous system injury or disease. The evidence supports ambulating on a treadmill at a rapid speed of 1.5 to 2.2 mph, with moderate to high intensity, and with assistance if needed. To meet these recommendations, a LiteGait body weight support system is utilized over its treadmills and over ground, according to Swingle. Some of the other specialty pieces of equipment that help make The Recovery Project different and help it gain referrals are the MyoPro device, Saebo, and Bioness H200, as well as VitalStim and the Red Cord Suspension System. TRP features an adaptable, open gym concept, with a group atmosphere where clients can encourage and motivate one another. Standardized performance measures are used to assess each patient’s progress, and data showing functional changes is shared with clients. “The majority of the clients we see have difficulty with mobility, or are in a wheelchair. Therefore, our equipment and facilities are adapted for these clients. Our FES RTI cycles can be utilized from a wheelchair. We also have the uppertoner strength machine that is accessible from a wheelchair, and we use MOTOmeds, which are also accessible to a wheelchair and provide a client with the ability to work on ROM, motor planning, and strengthening their arms or legs,” Swingle shares. Equipment used at TRP is chosen based on scientific evidence that it will benefit recovery, Swingle explains. “Due to the ever-changing environment of medicine, when we do purchase a piece of equipment, we look at the cost of updating the software or replacing the unit. We also look at the cost of repairs and replacement of parts due to the high utilization of these devices in our clinics. If available, we will trial a piece of equipment in our clinic for 3 months to determine its utilization and effects on recovery,” Swingle notes. RM





I am looking for equipment to assist me in gait having suffered a stroke.