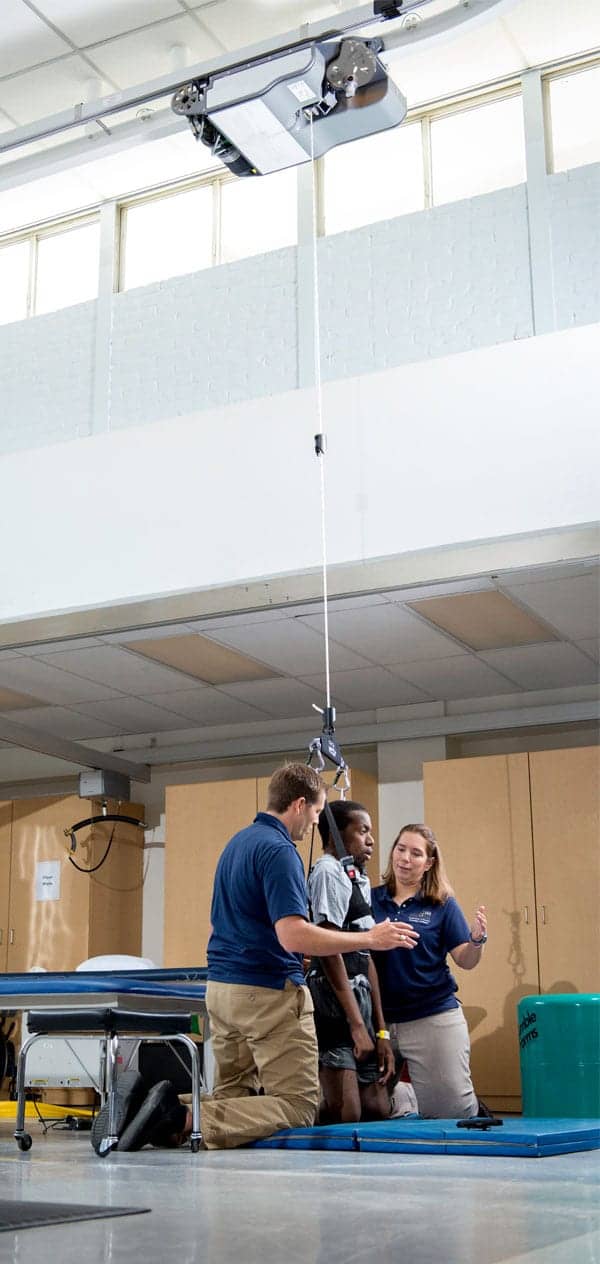
Body weight support systems confer several benefits to rehabilitation programs, including the ability to protect patients and therapists from fall-related issues, the ability for the therapist to focus on the patient’s tasks, and objective data that can be used to build patient motivation.
By Frank Long
Movement deficits in the lower extremities are not unusual in cases of stroke with drop foot, hemiplegia, and hemiparesis among the conditions commonly left behind. To battle these conditions rehab technology manufacturers are building and refining devices such as body weight support (BWS) systems, computerized balance systems, and integrated task systems. The technologies seem to have staying power and are proving their worth in stroke treatment programs. To learn more about how therapists are unfolding the benefits of these sophisticated tools, two therapists who use these technologies daily highlight the specific ways they help deliver results that optimize the effectiveness of therapy.
Made to Push the Envelope
“Our advanced technologies definitely do play a role as an adjunct to our traditional therapy,” says Audra Sturmoski, PT, stroke program coordinator for inpatient at The Rehabilitation Institute of St Louis (RISL). Sturmoski, a practicing therapist for 22 years, has worked at the 96-bed institute since it opened in 2001. Some of the advanced rehab technologies installed at the location include an over-treadmill body weight support system, a computerized balance system, and a computer-based integrated therapy system. These devices, Sturmoski says, deliver useful information for assessment by therapists that help dial in effective treatment.
Sturmoski considers the over-treadmill body weight support system at RISL one of the facility’s workhorses and says it is especially beneficial for those who work with patients who need a high level of physical assistance. She says the system provides the therapist the opportunity to control the speed of the patient’s gait more easily than if the therapist were walking with the patient over ground.
“For some of our patients the over-treadmill body weight support system actually makes them feel more comfortable because they don’t feel like they are depending on a therapist to hold them up,” Sturmoski says. “Instead, a very sturdy machine is holding up the patient, which makes that person feel more confident.”
Noting the growing popularity of BWS systems, Sturmoski says, nearly all of her colleagues in the area have access to some type of BWS technology.
Help from Above
Overhead track systems are another type of BWS system used with stroke and neurologic patients. These systems provide support to a patient who wears a harness attached by cable to a motorized trolley. The trolley, which can be operated via remote control held in the therapist’s hand, travels along a track installed in the ceiling. Samuel Uy, PT, uses an overhead track BWS system at Lakeland Regional Health, Lakeland, Fla. Uy says the technology provides stroke patients a more permissive environment where the therapist can do more to improve the patient’s plasticity.
“Using this system we can challenge patients more with their balance, pushing them more without the use of their assistive devices,” Uy says. “It improves their posture instead of relying on assistive devices, especially for those who use a cane and lean to one side and may eventually get into a habit of leaning to just one side.”
Uy adds that using the overhead track body weight support system helps those patients achieve more of an upright posture.
Information is an Adjunct One trend that seems to be catching on among BWS systems is the appearance of built-in features that collect real-time feedback and session data. These features are appearing throughout the market, from ceiling-mounted systems with six-figure price tags to more compact, harness-based movable systems that can be used over ground or over a treadmill.
The ability to capture information about weight bearing, balance, stride length, and speed not only makes treatment with these devices more accurate, but the use of those objective measures helps make progress “real” to patients more so than by using visual assessment alone.
In the case of the ceiling-mounted BWS system installed at Uy’s facility the system, he says, provides data he can show to a patient to demonstrate progress.
“For example, I can show a patient that in a previous session they had three falls and now they had only one fall. Or show them that previously their gait speed was .25 meters per second, and now the patient is doing .5 meters per second,” Uy says.
Having the ability to show data makes those individuals more appreciative of the results, Uy adds.
“In neuro rehab we call that ‘knowledge of result,’?” Uy explains. “That is especially good for neuro patients because once they see a good result based on objective findings rather than on subjective comments, they have a greater appreciation for their own progress.”
Uy adds that seeing the hard data motivates the patient more while doing therapy and can be especially helpful in motivating patients who are doing a complementary home program.
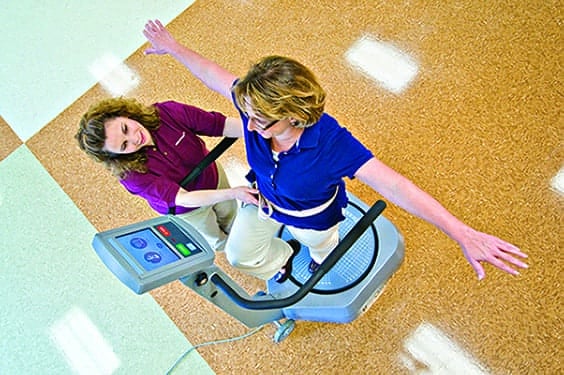
The story at RISL is similar, where Sturmoski says the power of objective data helps transform the idea of “progress” from abstract opinion to evidence-backed fact that the patient understands. The tool that most commonly provides this type of data at RISL, Sturmoski says, is a computerized balance system. The high-tech system features a platform with both static and dynamic balance capabilities and a touchscreen monitor to operate testing and training. It is shared among inpatient and outpatient departments, and has become so popular that careful scheduling is required to assure sessions do not overlap.
“One of the system’s features that we use most frequently is a basic measure that shows how much weight the patient is bearing on each limb,” Sturmoski says. “The therapist asks the patient to stand on it—that person may be a stroke patient who has weakness on the left side—and we’re trying to get them to bear more weight on their left side. The computerized balance system has a screen that shows where the weight is going and allows the patient to see that, yes, even though they feel like they are back in the middle, their weight actually is over on their right leg.”
The advantage of being able to use that objective data, Sturmoski says, is that it confirms what the therapist is telling the patients. As a result, the patient agrees that he or she needs to shift to the left side.
Motivational Effect of Task Training
An advanced rehab technology recently introduced by one manufacturer is an integrated therapy system that features an interactive touchscreen with a variety of program options. The device is offered by the manufacturer as a multi-disciplinary therapy solution that challenges the user with visual motor activities, among other types of training. The system provides data for standardized assessment to create an objective picture of progress for patients. One of these systems has been recently installed at RISL, where Sturmoski says its utility in treating the effects of stroke has caught on.
“We use it a lot with our speech and spatial neglect patients. In particular, we use the device’s program that allows us to look at a patient’s reaction time per quadrant on the screen of where they are hitting the targets. Using that program we can identify how slow the patient is to reach toward a certain quadrant and watch their progress over time,” Sturmoski says.
The same device is used by Uy and his colleagues. He describes it as a large video screen that engages patients in tasks that test hand-eye coordination and cognition.
“This system is particularly good because it provides lots of outcome measures, and I can rate the patient on how quickly he or she reacts to a certain stimulus or how good the coordination is,” Uy says.
Objective Measures of Gait
Electronic walkways are an example of another important device that can be used to generate objective measures for therapists to use. Among the providers of these technologies one manufacturer offers is a walkway built with a protective base, pressure sensor, and protective top on which assistive devices such as canes and walkers may be used. As many as 46,080 sensors are built into a pressure carpet for the purpose of capturing movement with high spatial resolution. Used with the manufacturer’s proprietary software, the walkway is able to output temporal, spatial, and pressure measures therapists can use in making static and dynamic assessments.
Gait mats, too, are tools that therapists can use to generate temporo-spatial data regarding a patient’s gait pattern. A gait mat developed by one manufacturer is built to provide exportable footfall, gait cycle, walk, and numerous other gait parameters to therapists. These devices, equipped with
imbedded sensors, are built for versatility in how and where they can be used. One manufacturer offers a model designed as sections that snap together as well as a range of portable options or units that can simply be rolled out and used in a hallway, flat ground, or on an incline.
Step therapy machines are also a technology that has been updated to provide data about therapy sessions. Some of these devices feature electronically elevating steps that can be customized to individual therapy sessions, with the steps on some devices engineered to rise from flat plane to more than 6 inches. Data about session date, time required to ascend and descend steps, and stair height can be collected and shared electronically. Another technology that has expanded its capabilities for stroke rehab is treatment and assessment platforms. More than simply providing utility as treatment tables, these platforms can be equipped with attachable parallel bars, electrically controlled adjustable backrests and seat lifts, and transfer bars. Some models are even designed to provide standing frame features.
The Road Ahead
As advanced technologies continue to emerge, they naturally will lay purchase decisions at the doorsteps of some decision-makers. Those decisions will require the evaluation of factors frequently at odds with one another, such as funding, cost-to-benefit ratio, and space constraints. Those factors will always matter where the healthcare economy is concerned. They loom less large, however, on the floor where therapists work to help patients reach their functional goals, especially when measured against the question: “What would the patient want?”
The answer to that question, in the context of what Sturmoski and Uy have observed, seems simple: what the patient wants is whatever will help them stand on their own two feet. RM
Frank Long is editorial director of Rehab Management.






Wow, the tool that measures where the weight is going sounds so helpful. I think my grandpa would really benefit from something like this.