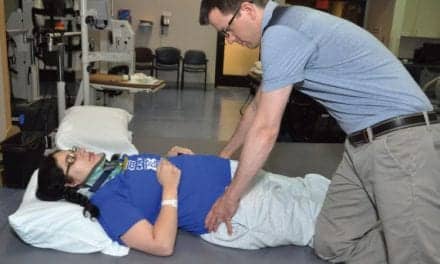
The stories each client and family has to tell are among the most valuable resources a clinician has in providing an optimum mobility solution.
by Susan Johnson Taylor, OTR/L (Editor’s note: This article provides a broad overview of concepts and thinking about clinical approach as well as current, detailed resources, told from the author’s point of view.) Mobility. This word means different things in different contexts. Usually, it represents moving from point A to Point B in the most efficient manner as possible, so that once at the destination, there is energy to participate. The International Classification of Function (ICF) assists us in defining a way of looking at the people with whom we work. First, there is a health condition (diagnosis), from which has associated impairments to the body’s structure (such as spasticity or contractures), which in some way limits the person’s activities (such as transferring), which in turn affects the person’s ability to participate in the manner they choose. As health care professionals in the field of complex rehabilitation technology (CRT), our job is to assess the impairments and limitations that affect a person, and apply some type of technology to address that individual’s desire to participate. In this case, it is to augment or completely replace the ability of the child to have self-initiated movement.
Childhood Development Waypoints
Where children’s development is concerned, the stakes are high. This is one of the issues and interventions that initially drew me to CRT, known as “technical aids” back then. As a newbie pediatric occupational therapist (OT) in Memphis, Tenn, in the early 1980s, my first job was at a place that no longer exists, but at the time was known as “The Crippled Children’s Hospital School.” Next door was the University of Tennessee Rehab Engineering program. In touring their building, I had never seen or even considered that such things as environmental control units, seating, or augmentative communication existed. They had a seating clinic at the hospital school and, since they had just lost their OT, asked if I would participate in their seating clinic. Having no idea what they were really talking about, I said, “sure.” And so it began. At the same time, led by Charlene Butler, an educator in Seattle and Karin Paulsson, a psychologist in Stockholm, Sweden, there was a lot of research into and talk about getting children mobile. There were presentations at Rehabilitation Engineering and Assistive Technology Society of North America (RESNA) conferences and the International Seating Symposium, which got all of us thinking about how we approached children and mobility. I went back to a pediatric textbook from OT school written by Barbara Banus and looked up typical development and what happens if something gets in the way of typical development. What I found included the following: • There is a critical time beyond which a given phenomenon may not appear….the longer the development is delayed, the more difficult it is to simulate….a wait and see attitude may waste valuable time • Child learns and tests limits, learns “no” • Learns about self in relationship to other people and objects • With these opportunities anger may appear overtly or covertly……likely to show anger, which is out of proportion to the event.1 It seemed so logical—of course, children need to move to develop, and do it as soon as possible. There are a number of researchers and clinicians who have spent a great deal of time connecting the need for self-initiated movement to development over the past 35 years or so, with a lot of the activity in the last 10 years. The need for and the cost of not having access to efficient mobility is well documented.
Family Matters
One of the most valuable things to a clinician are the stories each client and family has to tell. Each story accumulates into tribal knowledge that is passed on from clinician to clinician, and from clinician to family. These are powerful stories and testaments that what we try to do for the children with whom we work has a huge impact on participation. Mother after mother has related stories about being delighted that her child had an opportunity to misbehave or that now the child could actually play with friends. After being a clinician for several decades, the stories related to me have always guided and informed how I should speak with and introduce the idea of powered mobility to parents. Carol Schrader, mother of young adult triplets—two of whom are affected by cerebral palsy (CP) and use mobility devices, gave one of the best talks I have ever heard about her thoughts as her children grew up in a maze of therapists and therapies. Once she decided that the “W” word was not a bad word, she said something that I will never forget. “My boys are worth more than the sum total of their motor skills” (European Seating Symposium, Dublin, 2018; and International Seating Symposium, Pittsburgh, 2019; theblessingcounter.blogspot.com). Guiding students and new therapists along these lines is also very important.
Parents’ Perspective
Jill Marlow, OTD/S from Belmont University in Nashville, Tenn, was doing an internship with a complex rehab supplier headquartered in the Nashville area and was asked to write an article about parent’s perceptions of powered mobility. She was asked to not just focus on what the research said, but to really cue in on the interaction between the parent, therapist and supplier as they broached the subject. That is the part that allows us to understand the impact of what we are bringing up to a parent. Here is an excerpt from that article:
“One of the most impactful learning experiences I had involved this very topic (pediatric power). The ATP I was with gently brought up the topic of power to the parents of a child with mobility impairments. The ATP and therapist presented all of the benefits of powered mobility (PM) in a very optimistic manner, and described how it could directly and positively impact the child’s function. The parents immediately gave pushback on the idea and felt defeated at the thought of a powered wheelchair, saying that they were hopeful that their child would soon learn to walk. It would have been easy to present the evidence that PM does not hinder motor development, and aggressively push the idea on the parents. However, the ATP and the therapist acknowledged the parent’s thoughts, and listened to their concerns. They displayed empathy, understanding, and that acceptance of the idea may take time. It was apparent that the ATP and therapist left their personal judgments out of the conversation, and made an effort to understand the parent’s perception and address it appropriately. They used phrases such as, “this is what I’ve learned from other parents,” to help ease uncertainty.”
How Early is Too Early?
We understand that this is important. We know how to do this. We often get into the circle of: We have to wait until the children have developed skills to move independently—but to develop those skills, they need to move. Spearheaded by Cole Galloway, PhD, PT, at the University of Delaware, the Go Baby Go program was developed in 2012 to modify ride-on cars to get children moving. He was joined by Sam Logan at Oregon State in 2014 and Heather Feldner (now at the University of Washington). Efforts recently have been aimed at making this available to children who require it. In the article, “Why the time is right for a radical paradigm shift in early powered mobility: the role of powered mobility technology devices, policy and stakeholders,” Feldner states: “Advocacy efforts undertaken in partnership with families, clinicians, researchers, and disability communities are essential in recognizing mobility, and access to early powered mobility technology, as a human right.”2 Powered mobility is a powerful tool in the healthcare professional’s toolbox. Learning the history, understanding the stories, and enacting a plan as soon as possible that addresses the needs of the pediatric mobility user and family is of utmost importance to ensure an optimum long-term outcome. What is critical for therapists to remember is simply this: We have no time to waste.
Resources and reading recommended by the author of this article:
TEDx Talk, May 2015, “What I’ve Learned as a Childood Disability Doctor.” Lisa Thornton, MD, pediatric rehab medicine doctor at U of Chicago, available at YouTube.com. This presentation includes discussion about how children with disabilities versus typically developing children scored equally on how satisfied they were, no matter the severity of their disability. The speaker mentions that one factor that did lead to dissatisfaction was the lack of autonomy, being able to do things themselves and participate in decisions.
TEDMED Talk, 2014, “A Movement for Mobility, featuring Cole Galloway.” Available at YouTube.com.
Casey J, Paleg G, Livingstone R. Facilitating child participation through power mobility. Brit J Occup Ther. 2013;76(3):157-59.
Paulsson K, Christofferson M. Psychosocial effects on technical aids: how does independent mobility affect the psychological and intellectual development of children with disabilities? Journal of Early Intervention Theory and Practice. 2015;1(1).
Jones MA et al. Effects of power wheelchairs on the development and function of young children with severe motor impairments. Peds Phys Ther. 2012;4:131-40.
Free download from I-tunes https://itunes.apple.com/us/book/ready-set-go-powered-mobility/id991600558?mt=13
RESNA Pediatric Power Mobility Position Paper (11/2017): Compilation of expert opinion and summary of related research intended for education, reimbursement and to direct future research. Available at www.resna.org (under Knowledge Center)
Livingstone R, Paleg G. Practice considerations for the introduction and use of power mobility for children. Dev Med Child Neurol. 2014;56:210-221 Available at: http://onlinelibrary.wiley.com/doi/10.1111/dmcn.12245/pdf
Pituch E, et al. Powerful or powerless? Children’s, parents’ and occupational therapist’s perceptions of powered mobility. Phys Occup Ther Pediatr. 2019;39(3):276-291.
Kenyon LK, Mortenson WB, Miller WC. Power in Mobility: parent and therapist perspectives of the experiences of children learning to use powered mobility. Dev Med Child Neuro. 2018 Oct60(10).
Feldner H, Logan SW, Galloway JC. Mobility in pictures: a participatory photovoice narrative study exploring powered mobility provision for children and families. Disabil Rehabil Assist Technol. 2019 Apr;14(3):301-311.
Butler C. Augmentative mobility: why do it? Phys Med Rehabil Clin NA. 1991;2(4). • Banus B et al. The Developmental Therapist. Charles B. Slack: NJ 1979.
Feldner HA, Logan SW, Galloway JC. Why the time is right for a radical paradigm shift in early powered mobility: the role of powered mobility technology devices, policy and stakeholders. Disabil Rehabil Assist Technol. 2016 Feb;11(2).
Butler C. Effects of powered mobility on self-initiated behaviors of very young children with locomotor disability. Dev Med Child Neurol. 1986;28(3):325-332. RM
Susan Johnson Taylor, OTR/L, has been practicing in the field of seating and wheeled mobility for 38 years, primarily in the Chicago area at the Rehabilitation Institute of Chicago (now the Shirley Ryan AbilityLab) Wheelchair and Seating Center. She has published and presented nationally and internationally and is both a member of and fellow with RESNA. She is currently a member of the RESNA/ANSI Wheelchair Standards Committee and the Clinician Task Force. Taylor joined Numotion in 2015 as the manager of training and education. For more information, contact [email protected].
References 1. Banus B et al. The Developmental Therapist. Charles B. Slack: NJ 1979. 2. Feldner H, Logan SW, Galloway JC. Mobility in pictures: a participatory photovoice narrative study exploring powered mobility provision for children and families. Disabil Rehabil Assist Technol. 2019 Apr;14(3):301-311.
Mobility Goes Modern
by Frank Long, MS, Editorial Director
From the time of Confucius until about the middle of the 20th century, using a wheelchair was oftentimes a two-person task; especially for individuals with limited upper extremity strength and function who needed a second person to propel the wheelchair from behind. Those days ended abruptly in the 1950s when Canadian inventor George Klein introduced a power wheelchair considered practical for the consumer market. By today’s standards it was unwieldy and unattractive, but it opened the door for people affected by a mobility impairment to enjoy a new level of independence. The current market for adult power devices offers models with mid-wheel, front-wheel, and rear-wheel designs, which were inconceivable in the 1950s. Modern mid-wheel drive designs offer an extremely small turning radius useful for navigating indoor spaces. For those who need a device that will navigate uneven terrain or have a need to climb obstacles, a rear-wheel drive configuration offers the advantage of excellent stability. Another benefit of rear-wheel drive models is that they allow users to take advantage of higher drive speeds. A third type of design are front-wheel drives with independent suspension that can offer the user an extremely smooth ride. Having the large wheels located at the front of the wheelchair means when the device encounters an obstacle, the large wheels meet the obstacle first and typically are able to pull the rest of the wheelchair along. Aesthetics have also taken a giant stride forward from the look of Klein’s institutional metal tubing. The structural options wheelchair manufacturers have introduced to make today’s models more attractive and expressive include accent colors that can be used to personalize wheelchairs as well as shrouds that are built in a variety of distinctive colors and designs.
Seating and Positioning
Adjustability has made seating components and cushions nearly unrecognizable from what appeared in the 1950s. Seating frames for power wheelchairs are now engineered to be highly adjustable and can be combined with support options such as anti-shear backrests that reduce sliding between the cushion and the user, and flip-back armrests to help accommodate transfers. Power elevating legrests and other positioning products such as swing-away lateral thoracic supports, thigh supports, or knee supports are also modern options that help improve the power wheelchair user’s comfort and position. Modular custom seating technologies have also improved how therapists can approach the changing needs of wheelchair users with products engineered so they may be fitted and changed as the user’s shape, weight, or needs change. These custom seating products also can be useful for gradual corrective positioning and accommodate kyphosis, scoliosis, and lordosis. The flexibility they offer means they can be used to create low back, high back, and full body wheelchair seating. Customization is perhaps the unifying characteristic of modern seating solutions. This characteristic extends to seat cushions, which have evolved and become lighter as wheelchairs themselves have become more lightweight. Air and gel cushions, for example, offer lightweight performance but can redistribute pressure and reduce heat while protecting bony prominences. Gel and foam cushions, too, can provide good weight distribution, pressure relief, immersion, and envelopment without adding excessive weight. An alternating pressure cushion is an important development that has emerged especially for individuals at high risk of pressure sores. This cushion includes a built-in audio and visual alarm that is designed to warn the user about low pressure in the cushion. The cushion, which can be customized for each user, has coated foam on the exterior and features internal air bladders that automatically inflate and deflate. Tilt-in-Space technologies are another aspect of the mobility universe that have catapulted forward since Klein drew up his blueprints. These wheelchairs are engineered so an entire seating system may be tilted forward or backward while allowing the seat-to-back angle to remain constant. The modern tilt-in-space wheelchair is a useful mobility solution that can lower the risk of skin breakdown and improve the comfort of the wheelchair user. Their design offers additional benefits such as holding the head upright to improve the line of vision as well as facilitating feeding and respiratory function.
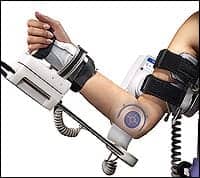
Drive Controls
Klein hardly could have foreseen how drive controls might evolve from the rudimentary joystick that appeared on his model. Advanced sip-and-puff technologies, tray arrays, and sophisticated head array systems fully integrated through an on-board CPU all work to provide users with an exceptional level of response and performance from their wheelchairs. That response, in turn, can improve the user’s own level of control and confidence in operating the device. And, as the personal technologies that wheelchair users use have evolved, so have wheelchair accessories. For example, in 1952 the market for Klein’s chair had no reason to make accommodations for cell phones or LED lighting. Today, however, not only are cell phone holders and LED lighting an option for users but so are conveniences such as underseat bags, armrest bags, protective canopies and cupholders. All of which assure that when wheelchair users leave home, they have a way to bring along their personal creature comforts safely and with style. RM