|
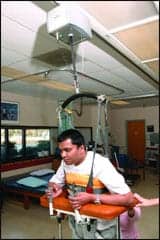
| Randy Ramnauth ambulates with a walker with a ceiling lift attached in case his legs buckle. The lift stabilizes him and prevents him from falling. |
The government projects 3 million new workers will enter the health care field by 2016—creating more new jobs than any other sector in industry. However, current Bureau of Labor statistics suggest those newly minted workers may become some of the most injury-prone employees in the nation: nursing homes rank a conspicuous third place for incidents of workplace injury.
The gloomy injury rates can potentially be improved, however, through wider adoption of available lift technologies designed to protect health care workers from the sometimes-hazardous nature of their own careers.
Back Injuries
Michelle Kerr, PT, is a therapist at Spaulding Rehabilitation Hospital, Boston Outpatient Center, and ranks back injuries as the most dominant injury among transport activities. A number of devices are available, including different types of patient lifts—manual, electric, or barrier-free—which Kerr says can be used to make it easier to perform transfers.
She also notes that while tasks such as bathing, toileting, or moving an individual in and out of a bed or vehicle can all present substantial risk to caregivers and clients, bathroom transfers are the most difficult maneuvers to perform.
“The bath/commode chairs are generally less stable surfaces,” Kerr says, “and the patients are usually wet and covered by less clothing than in other circumstances, which makes it much more difficult to move them safely.”
Kerr points out that the risk of injury for a caregiver or client is heightened particularly during transfer activities in home care situations, where caregivers are less well trained and fewer people are available to assist.
“Maybe only one caregiver is available to assist the client, and with some clients it can take two or three people to make transfers safe,” Kerr says. “Getting that many people to help is not always possible in a person’s private home.”
Adaptive Assistance
“Aging in place” is a functional living strategy supported by use of adaptive and assistive devices that is intended to allow mostly elderly individuals to remain in their homes, and stay out of skilled nursing facilities as long as possible—even as mobility declines. For home-based care, Kerr suggests professional caregivers who work for commercial care agencies often are better prepared to handle the risk of injury involved with limited mobility clients than a client’s family members, who may have had no experience dealing with such situations.
And though therapists and nurses typically train family members who will support the mobility needs of an individual returning home after a visit to a health care facility, Kerr says that the level of training can vary among different facilities.
Inside the home, assistive equipment issues become central in mobility strategies.
“Having appropriate equipment, and having that equipment properly set up, is also more optimal in the hospital setting,” Kerr adds. “Environmental issues with small bathrooms, doorway sizes, etc, can make mobility and transfers in the home more difficult, for both the client and the caregiver.”
Several affordable devices to smooth transport and positioning are available to caregivers in clinic or home settings, including circular pivot disks, which aid proper positioning. One-way glide cushions are available to prevent patients from sliding out of wheelchairs, and gait belts provide a level of safety for training activities or transferring patients by providing a secure way to grasp the patient.
Also available—and significantly more expensive—are electronic ceiling lifts, which can be used as fixed or portable transport solutions, and controlled remotely. The devices may also be used with walking slings to help ambulate patients more safely.
Lift and Transfer, Safely
Clients with bariatric requirements can make the already difficult challenges of lift and transfer downright daunting. Bariatric specialist Michael Dionne, PT, author of Lift Free Zone, points out that the decision by facility personnel to make a mechanically unassisted lift of a fallen patient heightens the risk of lift-related injury to workers while also potentially opening the door to a lawsuit brought by the patient in the event injury occurs during the manual lift.
In such circumstances, Dionne states, the mechanical lift becomes the technique of choice.
“Today, any caregiver should be able to use a mechanical lift to transfer a patient, no matter how dependent that patient is,” Dionne notes in an earlier interview with Rehab Management.
Individuals who are “medically fragile,” also have special concerns that should be met to assure safe transfer activities between caregiver and client. Anne Kilpatrick Lorio, MSPT, Multi Specialty Care Unit, Shepherd Center, Atlanta, recommends the SAFE method for transfers to minimize risk of injury to caregiver and patient. This method comprises the following steps:
- Secure the patient and environment. If using a sling or net, make sure the device is placed appropriately beneath the patient. Confirm that the lift being used is secure and in good working order. Lift devices in a health care setting should be inspected frequently by the biomedical department. Check for cracks or loose parts. Only devices that have been cleared for use with the patient should be used. The beds, chairs, or carts used for patient transfer should all be locked before the patient is moved. Confirm patient does not exceed device’s weight limit.
- Ask for help if it is needed, particularly for clients who are large or difficult to transfer
- Fully inspect the transfer area before you do the transfer—the environment should be clear of hazards or clutter. If the client is attached to a ventilator or has a Foley catheter or other tubing attached, assign someone to be in charge of the tubing to assure nothing pops off or is pulled from the patient.
- Education is key for safe transfers. Lift operators should clearly understand how to use the device in all situations. Educate clients so they can verbalize all the appropriate transfer steps.
Frank Long is the associate editor of Rehab Management. For more information, contact .
The Benefits of Lift Technology
by Sharon Brumbeloe, RN
There are multiple benefits to both caregiver and client provided by lift and transfer aids, including:
- Staff Retention—especially experienced staff. The addition of technical aids helps keep experienced professionals on the job. Keeping any employee—particularly experienced PTs, OTs, and RNs—means higher quality patient care, improved outcomes, and cost savings. According to some human resource consultants, the recruitment, screening, hiring, and orientation of new employees can exceed several thousand dollars.
- Recruitment—Newly trained health care professionals are technologically savvy and will work only where administrative commitment, policies, and equipment offer them maximum success for a long career. These new professionals are looking for technical aids.
- Efficiency—Staff work more efficiently and effectively when they can perform the patient task immediately without waiting for one, two, or even three additional caregivers to come.
- Patient Satisfaction—Patients say they feel safer and more comfortable in a lift hammock/sling.
- Employee Satisfaction—Employees say, “This is a great place to work because they really care about me and give it more than lip service; they prove it with the addition of technical aids.”
- Reduced Costs—Costs due to employee sick days and light-duty days are reduced immediately when safe lifting policies and technical aids are available.
- Reduced Compensation Claims—Workers’ compensation costs have been reduced in some cases by 35% to 65%. Repositioning patients in beds and transfers from bed to chair cause most of the injuries to caregivers across this country. PTs and OTs are often called on to help nurses with these two types of transfers because, according to the nurses, “these professionals know how to do it right.” However, age, strength, and sex are irrelevant when calling for assistance—the issues are the same: a health care worker’s back will sustain irreversible injury over time if they repeatedly lift patients, or they must place their own backs in an awkward position to lift a patient.
- Reduced Patient Falls—Adding lift technology significantly reduces the number of potentially injurious patient falls.
The Joint Commission on Accreditation of Healthcare Organizations and other professional reviewing entities look favorably on a well-defined, system-wide program of lifting devices and training. •
Sharon Brumbeloe, RN, is a registered nurse with experience working in rehab, critical care, hospice, and assisted living settings. She currently works at Oklahoma Heart Hospital, a specialty hospital, in Oklahoma City. For more information, contact [email protected].