Blending dedication and technology helps bring mobility goals into focus for patients who have sustained stroke or spinal cord injury.
Injuries to the nervous system can be devastating, and much uncertainty exists as to how much function the patient will recover. This is true for injuries to the brain, such as stroke, and injuries to the spinal cord. When a patient arrives at Burke Rehabilitation Center, a 150-bed acute care hospital in White Plains, NY, after having suffered a stroke or a spinal cord injury (SCI), their care is coordinated in a multidisciplinary, team-based approach. A care team consists of a physician, nurse, physical therapist, occupational therapist, speech therapist (if applicable), as well as a social worker, recreation therapist, respiratory therapist, nutritionist—and, of course, the patient and caregiver. This model of care allows all team members to work collectively, engaging the patient in a minimum of 3 hours of one-on-one therapy up to 6 days per week. As the patient makes strides toward recovering ambulation or learning to use adaptive techniques for mobility, the team can utilize various technologies and equipment to enhance the patient’s strengths and help them recover to the fullest extent possible.
EVALUATING THE PATIENT
Upon admittance to the facility, each patient receives an initial evaluation. The team of physicians, nurses, and therapists looks at the level of impairment and functional limitations the patient may have, including their strength, balance, range of motion, and sensation. This evaluation, paired with the patient’s medical diagnosis from their referring hospital, allows the team to create a plan of care and set functional goals.
For patients affected by a spinal cord injury, the physician will perform the International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) examination1 to determine the extent of the patient’s injury and provide an impairment scale, known as the ASIA impairment scale. There are five levels of impairment, which are ranked from A to E, and based largely on statistics from the past 20 years. Level A is a complete injury, with statistics indicating that only about 1% of patients will walk by the end of 1 year, while level D indicates that about 90% of patients with this level of impairment will walk by the end of 1 year. Determining this information allows the physician to predict fairly accurately what the goals will be for ambulation.
For stroke patients, a complete neurological exam, including a motor evaluation, is administered. The physician will check the patient’s strength and reflexes and determine whether they can sit and stand, as well as assess whether the patient can take any steps. The physician also will test for presence of increased muscle tone, which can often occur after stroke. Sometimes, increased muscle tone can get in the way of ambulation, since it can make it difficult to straighten the leg and causes the muscles to develop resistance. These exams set the stage for the physicians and therapists to pinpoint how and where the various equipment can help a patient become more mobile.
SETTING GOALS
Once the patient has been given the initial assessment, the team will work together, including the patient and family, to create a series of goals. Setting goals can take a two-pronged approach. The first are goals for the short term, such as how much can be accomplished in a week. The second are goals for the long term, such as the overall goals for the patient’s length of stay. These goals can then be revised as the patient progresses, as the team meets to discuss the progress of every patient on a weekly basis or, if necessary, more frequently.
For a stroke patient, for example, the first functional goal might be to increase bed mobility, which can help prevent development of pressure ulcers. The next goal might be for the patient to transfer from the bed to either the wheelchair or the commode. Once that goal is met, the next goal may be ambulation. Initially, the team may simply work on helping the patient stand upright, holding onto a bar or the therapist, if necessary. Eventually, through the use of technology such as custom-made treadmills with a body-weight support (BWS) system, and lower extremity functional electrical stimulation (FES) rehab devices engineered to combine electrical stimulation and orthotic technology, the patient can begin to utilize functional movement.
The goal for most patients, both those who are nonambulatory as well as those who are ambulatory with a specific amount of assistance, will be to walk again. For those with severe limitations, the goals may differ. Burke’s goal is for each patient to reach the maximum level of independence. The important thing for physicians and therapists to remember is not to discourage the patient from trying to achieve this goal, but to balance it with realistic expectations. Furthermore, the therapist and physician must remember it is important for the patient to understand that being dedicated to rehab and working as hard as possible can have particularly positive effects.
With spinal cord patients, for instance, much of the original assessment is driven by established statistics. But while these statistics might be quite accurate, there is always a small chance for patients to exceed their expected recovery and potentially achieve ambulation. The most important point is that a therapist or physician will never know whether that patient is going to be among that small percentage unless they try—both through the use of BWS-based treadmill training, and through the patient’s own dedication to rehab.
A recent stroke patient, for example, was told she had no rehabilitation potential, but her family fought to have her admitted to Burke. Although she had no movement when she arrived, after being at the hospital for 3 weeks, she became able to sit in her wheelchair, attempted to form words, and—with assistance—able to transfer a ball from one hand to another. Every patient is unique, but with the correct type of rehabilitation, use of technology, and dedication (by patient and rehabilitation team), the patient often makes significant strides.
USING TECHNOLOGY
While setting goals and assisting the patient in meeting and hopefully exceeding them is important, in today’s advancing medical landscape, the use of technology is an essential step in helping a patient achieve maximum recovery—especially as it relates to ambulation. The use of these technologies offers multiple benefits. In the past, therapists relied on the utilization of body mechanics and physical support to help a patient become more mobile. If a stroke patient was completely nonambulatory, a therapist would maneuver the patient’s frame while other therapists would move each of the patient’s legs in order to stimulate movement.
Today, the use of technology such as BWS treadmill training systems can help alleviate the physical burden to the therapist. These types of treadmills can be used for ambulatory and nonambulatory patients. A specific type of body-weight support treadmill was custom-built for Burke, in which the patient is placed in a harness over a treadmill that supports the body’s weight as the patient moves, and positions the legs when attempting ambulation.
The therapist can identify an appropriate amount of support to provide the patient using the system by looking at their ability to maintain upright posture and ability to step. The amount of support can be easily adjusted during a session and from session to session to provide the greatest amount of challenge to the patient’s system, while also optimizing their kinematics. This system allows therapists to assist patients in upright weight-bearing activities early on in the recovery process in a safe and dynamic environment. The technology provides the opportunity to make real-time changes and adjustments during weight-bearing and gait activities throughout a patient’s length of stay while allowing therapists to track the progress of an individual’s ability to support their own body weight, maintain upright posture, and take steps. The goal is always to use the system to eventually translate to movement over ground with or without support or assistance.
These systems also offer another important technological purpose: the importance of repetition. For example, with only 20 minutes on the treadmill, a patient affected by a spinal cord injury is able to take many more steps than they would if only using a harness over the ground. While the exact underlying mechanism for this remains unclear, one theory is that the repetition helps to repair existing but injured connections in the spinal cord circuitry (compared to new connections being established).
While studies have shown varied results from using the treadmill with an SCI patient, a study conducted at the University of Leeds published in 2011 notes, “The most effective way of restoring locomotion is through complete repair; however, regeneration techniques are still being developed. For regeneration to take place, the neurons within the spinal cord that are important in generating rhythmic movements (the central pattern generator [CPG] circuits) still need to be functioning, as these circuits have been shown to decline through long periods of inactivation. Treadmill training has therefore an important role in keeping neurons active until regenerative techniques become viable.”2
After stroke, animal studies have shown that animals can improve, but the studies were tracking hundreds and thousands of movement repetitions. While the same number of repetitions wouldn’t necessarily be able to be replicated in humans, simply utilizing these technologies allows for an increase in repetition when compared to the number of reps a patient could do without the equipment. This will hopefully help to improve outcomes.
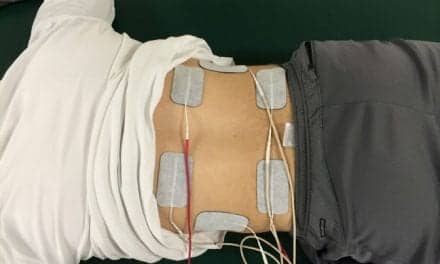
Treadmills are not the only effective technology in helping build repetition during a patient’s rehab. The use of electrical stimulation in the clinic has been equally important in recovery and keeping the body prepared for movement during the recovery process. Bicycles with FES, which allow for cycling with either arms or legs while the patient sits, and can be used for lower extremity strength and conditioning, are timed to release a small amount of electrical stimulation where and when the muscles would normally fire. This allows physicians and therapists to see exactly how much force is driven by the patient’s muscles and how much is driven by the electrical stimulation, allowing them to adjust their techniques as needed.
Another benefit of the FES bikes is their help in preventing muscle atrophy and strengthening weak muscles. If a semiambulatory patient does regain full use of the legs, those muscles will be ready to work. For nonambulatory patients, the bikes also help maintain circulation and overall health.
The technology can have peripheral benefits as well. For both ambulatory and nonambulatory patients, the simple act of standing using a BWS treadmill training system or a partial-weight-bearing gait therapy device, a harness system in use at Burke, can help with bowel and bladder function, to correct blood pressure dysfunction, and to increase endurance.
Another benefit of using this technology that can have a long-lasting impact on a patient’s recovery: the psychological aspect of seeing the legs and feet move. Naturally, it can be difficult for patients to come to terms with the fact that they may not walk again—or walk in the same way they did before a stroke or spinal cord injury. But for patients to simply see the movement that they are able to create using these technologies can help them to continue moving forward. It can help make the goals established at the beginning of therapy and throughout the rehabilitation program seem more tangible and feasible. Perhaps most importantly, however, it can help the patient stay positive in the face of a life-changing event. RM
Argyrios Stampas, MD, is the director of Burke Rehabilitation Hospital’s Spinal Cord Injury Rehabilitation Program. He has specialized experience and certification from the American Board of Physical Medicine and Rehabilitation in the treatment of patients with spinal cord injuries. Dr Stampas is a graduate of the State University of New York Upstate Medical University and completed his residency at the University of Pennsylvania in physical medicine and rehabilitation. He completed his subspecialty in Spinal Cord Injury at Johns Hopkins Hospital.
Carolin Dohle, MD, is an attending neurologist for Burke Rehabilitation Hospital’s Stroke Rehabilitation Program and is certified by the American Board of Psychiatry and Neurology and the American Board of Integrative Holistic Medicine. Dr Dohle also serves on the Clinical Trials Task Force of the American Society for Neurorehabilitation (ASN), where she is also a member. She earned her doctorate from Ruhr University Bochum in Bochum, Germany, and completed her Neurology training at Yale University School of Medicine. She is currently working toward an advanced certificate in clinical investigation at Weill Cornell Medical College in New York City.
Elizabeth Dominick, PT, DPT, NCS, is the clinical team leader of Burke’s Spinal Cord Injury Rehabilitation Program. She received her initial degree in Physical Therapy from Ithaca College and her transitional Doctorate in Physical Therapy from Boston University. Dominick is a Board Certified Clinical Specialist in Neurologic Physical Therapy and has been with Burke 12 years. For more information, contact [email protected].
References
1. http://www.asia-spinalinjury.org/elearning/ISNCSCI.php
2. http://biohorizons.oxfordjournals.org/content/4/1/108.abstract